🚨 Acute Kidney Injury (AKI)
🔹 Definition
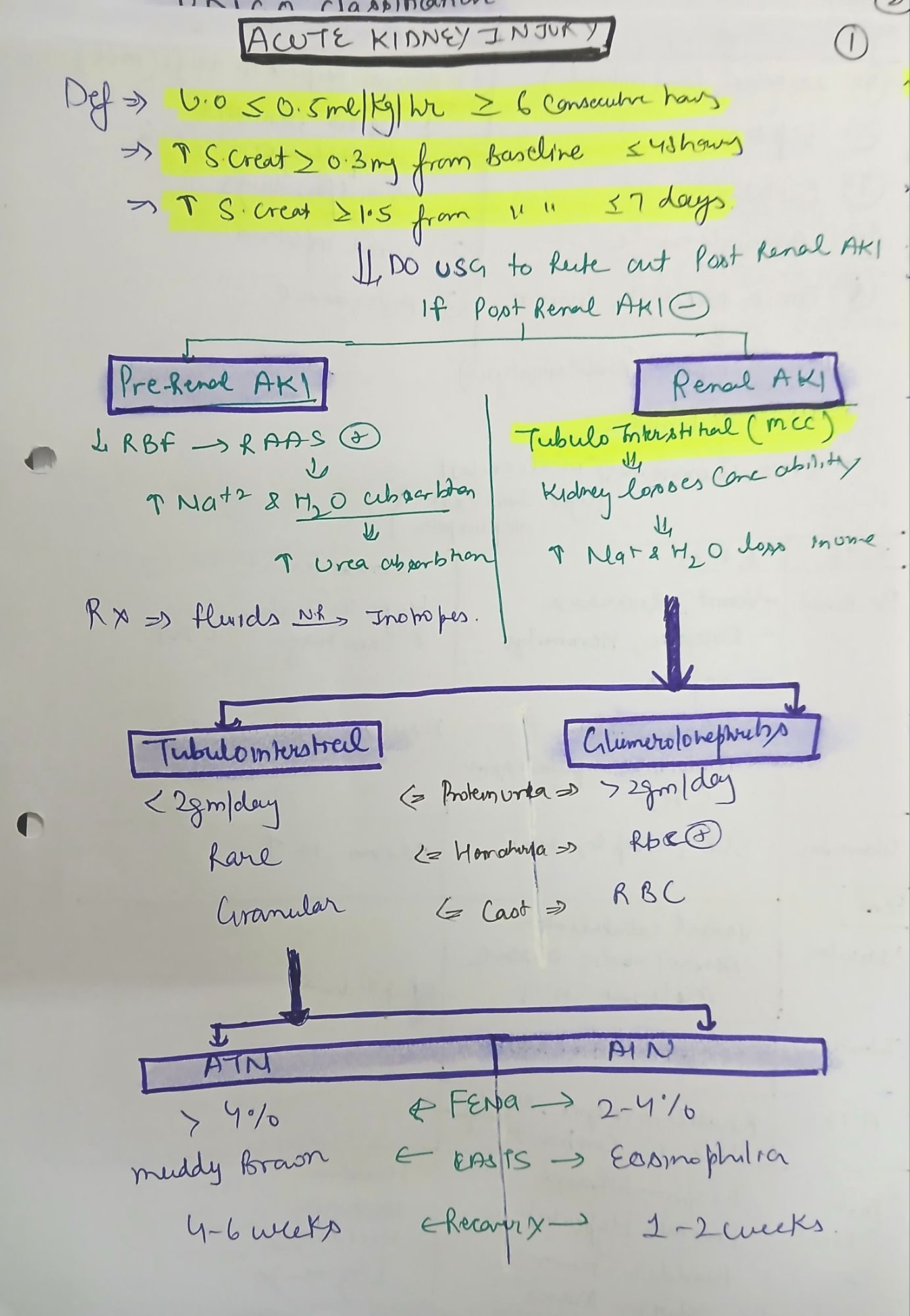
AKI is a rapid decline in kidney function (hours to days), resulting in the accumulation of nitrogenous waste, electrolyte imbalance, and dysregulation of volume and acid-base status.
🔬 KDIGO Criteria (Most widely used)
AKI is diagnosed if any of the following are present:
- ↑ Serum creatinine (SCr) by ≥0.3 mg/dL within 48 hours
- ↑ SCr ≥1.5× baseline within 7 days
- Urine output (UO) <0.5 mL/kg/h for ≥6 hours
KDIGO Staging
|
Stage |
Creatinine Criteria |
Urine Output |
|
1 |
1.5–1.9× baseline or ↑ ≥0.3 mg/dL |
<0.5 mL/kg/h for 6–12 h |
|
2 |
2.0–2.9× baseline |
<0.5 mL/kg/h for ≥12 h |
|
3 |
3.0× baseline or SCr ≥4 mg/dL or RRT needed |
<0.3 mL/kg/h ≥24 h or anuria ≥12 h |
📊 Etiological Classification
|
Type |
Mechanism |
Common Causes |
|
Pre-renal |
↓ Renal perfusion |
Hypovolemia, shock, heart failure, NSAIDs |
|
Intrinsic |
Renal parenchymal damage |
ATN, glomerulonephritis, AIN |
|
Post-renal |
Obstruction of outflow |
Stones, BPH, catheter kink, tumor |
🔍 Pathophysiology in ICU
- Ischemia, sepsis, toxins → tubular cell injury → ATP depletion → cell death
- Tubular obstruction by debris (cast formation)
- Endothelial injury, microvascular dysfunction
- ↑ Inflammatory cytokines → systemic complications
🔬 Diagnostic Workup
|
Investigation |
Use |
|
Urine output & trends |
Early marker |
|
Serum creatinine, BUN |
Diagnostic and staging |
|
Urine sodium, FeNa |
Distinguish pre-renal (<1%) from ATN (>2%) |
|
Urinalysis, microscopy |
Muddy brown casts → ATN; eosinophils → AIN |
|
Renal USG |
Rule out obstruction (post-renal) |
|
Biomarkers (optional) |
NGAL, KIM-1, IL-18 (early detection) |
🧠 Key ICU Principles
✅ 1. Fluid Resuscitation
Goal: Restore perfusion in pre-renal/early AKI (esp. in sepsis)
Logic:
- Hypovolemia → ↓ renal blood flow → ischemic injury
- Resuscitation reverses pre-renal AKI and prevents ATN
Preferred fluid:
- Balanced crystalloids (Ringer’s lactate, PlasmaLyte)
- Avoid high chloride (NS) → renal vasoconstriction
Dosing:
- Initial bolus: 500–1000 mL over 15–30 min
- In sepsis: 30 mL/kg (Surviving Sepsis Campaign)
Caution: Avoid fluid overload (↑ mortality in AKI/ARDS)
✅ 2. Vasopressors
Why: To maintain renal perfusion pressure when fluids insufficient
First-line:
- Norepinephrine: 0.05–0.5 mcg/kg/min (target MAP ≥65 mmHg)
Alternatives:
- Vasopressin: 0.03 units/min if NE insufficient
- Angiotensin II (in refractory vasodilatory shock; costly)
Logic: Hypotension → ↓ GFR → ischemic AKI. Maintaining MAP helps autoregulation.
✅ 3. Avoid Nephrotoxins
- Drugs: Aminoglycosides, vancomycin, amphotericin B, contrast, NSAIDs
- Adjust all drug doses based on eGFR/CrCl
Use renal-safe antibiotics:
- Cefepime, meropenem, adjusted to renal function
✅ 4. Electrolyte & Acid-Base Management
|
Issue |
Management |
|
Hyperkalemia |
Calcium gluconate 10 mL IV, Insulin + Dextrose, furosemide, dialysis |
|
Metabolic acidosis |
NaHCO₃ if pH <7.1 or bicarb <12 |
|
Volume overload |
Loop diuretics (furosemide), RRT |
✅ 5. Diuretics (for volume control only)
- Furosemide: 20–80 mg IV bolus or continuous (e.g., 5–10 mg/h)
- May help in oliguric AKI with fluid overload
- Do not improve survival or prevent RRT need
✅ 6. Renal Replacement Therapy (RRT)
Indications: “AEIOU” mnemonic:
- A: Metabolic Acidosis (pH <7.1 refractory)
- E: Electrolyte imbalance (K⁺ >6.5 mmol/L or refractory)
- I: Intoxications (e.g., lithium, methanol, salicylates)
- O: Volume Overload (pulmonary edema, unresponsive to diuretics)
- U: Uremia (e.g., pericarditis, encephalopathy)
Modes:
- Intermittent HD: Hemodynamically stable patients
- CRRT (CVVH, CVVHDF): Preferred in ICU/septic shock
- Dose: 20–25 mL/kg/hr (effluent flow)
- SLED: Hybrid between intermittent HD and CRRT
Timing:
- Controversial – current trend: “wait for indications”
- ELAIN trial favored early initiation
- AKIKI trial showed no benefit with early RRT
✅ 7. Nutrition in AKI
- Avoid overfeeding
- Protein: 1.2–1.5 g/kg/day (↑ in RRT: 1.5–2 g/kg/day)
- Monitor electrolytes (esp. K, Phos) closely
📋 Summary Table: ICU AKI Management
|
Intervention |
Rationale |
Doses / Notes |
|
Fluids |
Restore perfusion |
Balanced crystalloids, 500–1000 mL bolus |
|
Norepinephrine |
Maintain MAP ≥65 |
0.05–0.5 mcg/kg/min |
|
Diuretics |
Volume control only |
Furosemide 20–80 mg IV |
|
RRT |
AEIOU indications |
CRRT preferred in ICU |
|
Avoid nephrotoxins |
Prevent further injury |
Adjust all nephrotoxic meds |
|
Electrolyte correction |
Prevent arrhythmia/metabolic derangement |
IV calcium, insulin, bicarbonate as needed |
🧠 Special ICU Situations
|
Condition |
AKI Link |
|
Sepsis |
Most common ICU AKI cause (SA-AKI); inflammatory + ischemic |
|
Rhabdomyolysis |
Myoglobin-induced ATN; aggressive hydration, alkalinize urine |
|
Cardiorenal Syndrome |
Low CO → ↓ GFR; treat heart failure, cautious diuresis |
|
Hepatorenal Syndrome |
Splanchnic vasodilation; treat with Terlipressin + albumin |
🧪 Renal Biomarkers (Research/Early Detection)
|
Biomarker |
Use |
|
NGAL (Neutrophil gelatinase-associated lipocalin) |
Early AKI detection |
|
KIM-1, IL-18, Cystatin C |
Ongoing research |
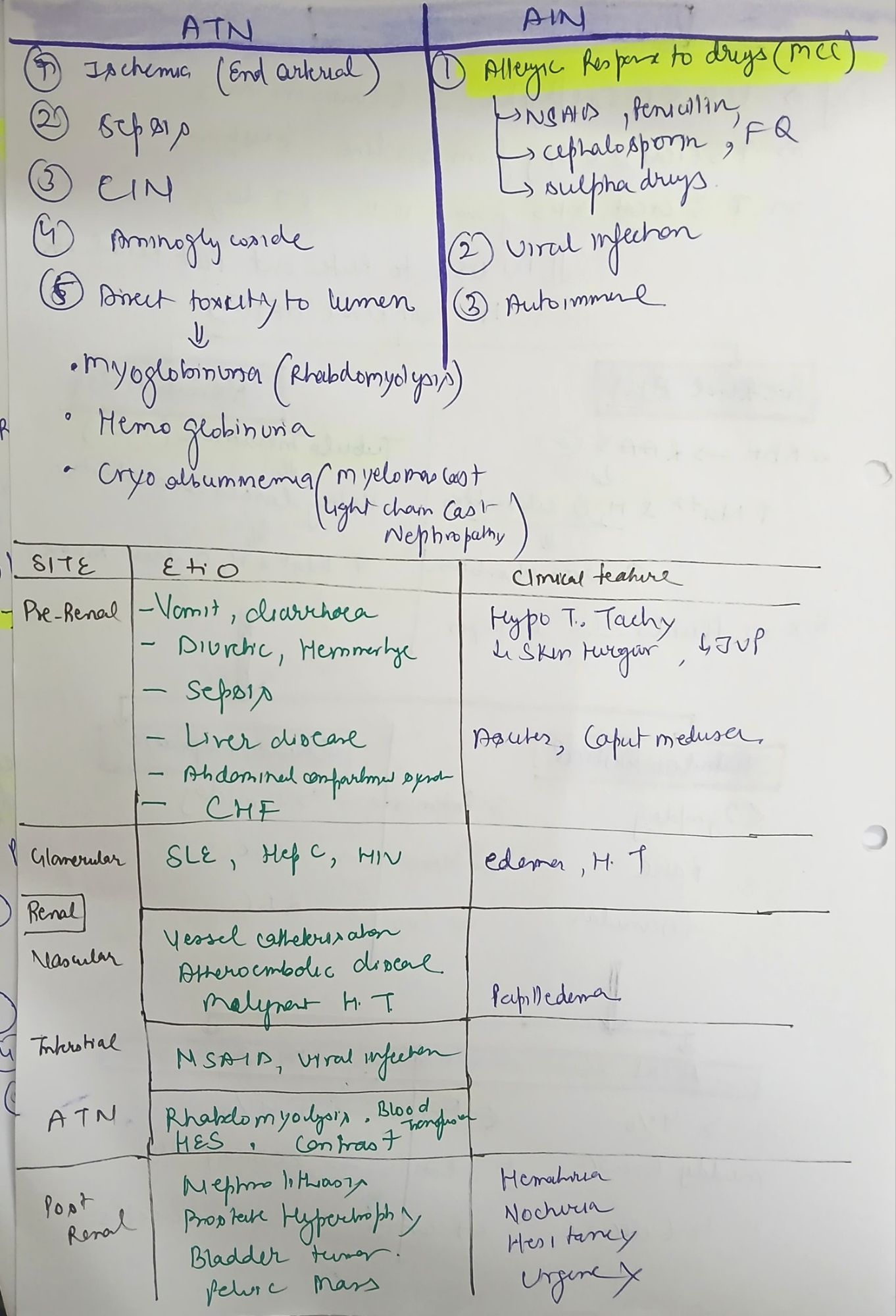
🔍 AIN vs ATN: Differentiating Two Common Causes of Intrinsic AKI
🧠 Overview
Both ATN and AIN are causes of intrinsic acute kidney injury (AKI) but differ in pathophysiology, etiology, clinical presentation, urine findings, and management.
📊 Comparison Table: AIN vs ATN
|
Feature |
Acute Interstitial Nephritis (AIN) |
Acute Tubular Necrosis (ATN) |
|
Site of Injury |
Interstitial tissue ± tubules |
Tubular epithelial cells |
|
Common Causes |
– Drugs (70–90%): NSAIDs, β-lactams, PPIs, rifampin, diuretics – Infections: CMV, EBV, TB – Autoimmune: SLE, Sjögren |
– Ischemia: sepsis, hypotension, surgery – Nephrotoxins: aminoglycosides, contrast, myoglobin, cisplatin |
|
Onset |
Subacute (days–weeks) |
Acute (hours–days) |
|
Classic Triad (seen <10%) |
Fever, rash, eosinophilia |
None |
|
Urine Output |
Often non-oliguric |
Often oliguric (<400 mL/day) |
|
Urine Findings |
– WBCs, WBC casts – Eosinophiluria (Hansel stain) – Mild proteinuria |
– Muddy brown granular casts (classic) – Epithelial cell casts – No eosinophils |
|
FeNa (%) |
Variable; often <1% (but not reliable) |
Typically >2% (unless on diuretics) |
|
Serum Findings |
↑ Cr, ↑ eosinophils (50–80%) |
↑ Cr, ↑ BUN |
|
Kidney Biopsy |
Interstitial edema, infiltrates (lymphocytes, eosinophils) |
Tubular cell necrosis, loss of brush border |
|
Treatment |
Stop offending drug ± Steroids: Prednisone 1 mg/kg/day x 1–2 weeks, taper |
Supportive care Maintain perfusion RRT if needed |
|
Prognosis |
Usually recovers if identified early |
Recovery possible, but slower |
💡 Key Differentiators in ICU
|
Clue |
Suggests |
|
Rash + fever + eosinophilia |
AIN |
|
Recent antibiotics / NSAIDs |
AIN |
|
Sepsis + hypotension |
ATN |
|
Nephrotoxic drug (e.g. gentamicin) |
ATN |
|
Muddy brown casts |
ATN |
|
Eosinophiluria |
AIN (but not specific/sensitive) |
📌 When to Biopsy?
Indicated when:
- Cause unclear
- No improvement despite supportive care
- Suspected AIN (for steroid decision)
- Rapidly progressive renal failure
🧠 1. RIFLE Criteria (2004 – by ADQI group)
RIFLE is an acronym:
|
Stage |
Meaning |
|
R |
Risk |
|
I |
Injury |
|
F |
Failure |
|
L |
Loss (persistent failure >4 weeks) |
|
E |
ESRD (failure >3 months) |
🔢 RIFLE Staging (based on GFR or Creatinine + Urine Output)
|
Class |
Creatinine/GFR Criteria |
Urine Output Criteria |
|
Risk |
↑Cr ×1.5 or GFR ↓ >25% |
<0.5 mL/kg/h for 6 h |
|
Injury |
↑Cr ×2 or GFR ↓ >50% |
<0.5 mL/kg/h for 12 h |
|
Failure |
↑Cr ×3, Cr >4.0 mg/dL (acute rise ≥0.5) or GFR ↓ >75% |
<0.3 mL/kg/h for 24 h or anuria for 12 h |
|
Loss |
Persistent renal failure >4 weeks |
— |
|
ESRD |
End-stage kidney disease >3 months |
— |
🧠 2. AKIN Criteria (2007 – Acute Kidney Injury Network)
- Modified and simplified RIFLE
- Removed GFR criteria (hard to measure acutely)
- Added absolute rise in creatinine ≥0.3 mg/dL
- Must occur within 48 hours
🔢 AKIN Staging
|
Stage |
Creatinine Criteria |
Urine Output |
|
Stage 1 |
↑ ≥0.3 mg/dL or 1.5–2× baseline |
<0.5 mL/kg/h for ≥6 h |
|
Stage 2 |
↑ 2–3× baseline |
<0.5 mL/kg/h for ≥12 h |
|
Stage 3 |
↑ >3× baseline or ≥4.0 mg/dL (with rise ≥0.5) or dialysis required |
<0.3 mL/kg/h for ≥24 h or anuria ≥12 h |
🚨 Phases of Acute Kidney Injury (AKI)
📌 Overview
AKI is characterized by rapid decline in renal function, with or without oliguria, leading to azotemia, fluid/electrolyte imbalance, and acid–base disorders.
AKI typically progresses through four sequential phases, though some may be absent or overlap.
🔄 1. Initiation Phase
- Duration: Minutes to hours
- Trigger: Insult causing decreased renal perfusion or direct tubular injury
- Examples:
- Hypotension, sepsis, nephrotoxins, rhabdomyolysis
- Events:
- ↓ GFR
- ATP depletion in tubular cells
- Endothelial dysfunction
- Subclinical injury may be occurring before serum creatinine rises
📌 Potentially reversible if insult is corrected promptly
⛔ 2. Oliguric/Anuric Phase
- Duration: Days to 1–2 weeks (sometimes longer)
- Urine output: <400 mL/day (oliguria), or <100 mL/day (anuria)
- Events:
- Tubular epithelial cell necrosis and sloughing
- Intratubular obstruction and backleak of filtrate
- GFR remains low
- Complications:
- Volume overload
- Hyperkalemia
- Metabolic acidosis
- Uremia → encephalopathy, pericarditis
- Hyponatremia, hyperphosphatemia
🔬 Labs: Rising BUN, creatinine; hyperkalemia; low Na⁺ and HCO₃⁻
💧 3. Diuretic (Polyuric) Phase
- Duration: Days to weeks
- Urine output: Often >3–5 L/day
- Mechanism:
- Regeneration of tubular cells begins
- Tubular dysfunction persists: can’t concentrate urine or reabsorb Na⁺/water
- Osmotic diuresis due to accumulated urea and solutes
- Consequences:
- Polyuria, despite persistent azotemia
- Electrolyte loss: K⁺, Na⁺, Mg²⁺ → hypokalemia, hypovolemia
- Hypotension
⚠️ ICU patients may need aggressive electrolyte and volume replacement
🛠️ Why Polyuria Happens (Mechanism)
- Tubular epithelial cell regeneration: starts → tight junctions not fully functional
- Loss of concentrating ability: impaired medullary gradient, dysfunctional Na⁺/K⁺/Cl⁻ cotransporters
- Osmotic diuresis: from urea, retained solutes
- Impaired ADH responsiveness: temporarily
- Increased GFR but poor reabsorption → high-volume dilute urine
🟢 4. Recovery Phase
- Duration: Weeks to months
- Events:
- Gradual restoration of normal tubular function
- GFR returns toward baseline
- Urine output normalizes
- Complete recovery possible, but:
- May have residual CKD, especially if older, multiple comorbidities
- Some may develop progressive renal fibrosis → ESRD
🧠 ICU Clinical Implications
|
Phase |
Clinical Action |
|
Initiation |
Prevent further insult: hemodynamic support, avoid nephrotoxins |
|
Oliguric |
Dialysis if needed (based on AEIOU), manage fluid/electrolytes |
|
Polyuric |
Monitor urine output hourly; replace losses; watch for arrhythmias (hypokalemia) |
|
Recovery |
Monitor creatinine trends; adjust medications as function returns |